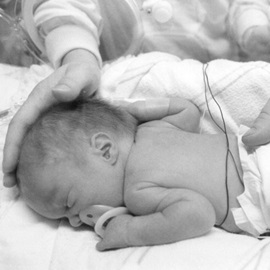
St. Luke’s NICU baby to NICU caregiver: a nurse comes full circle
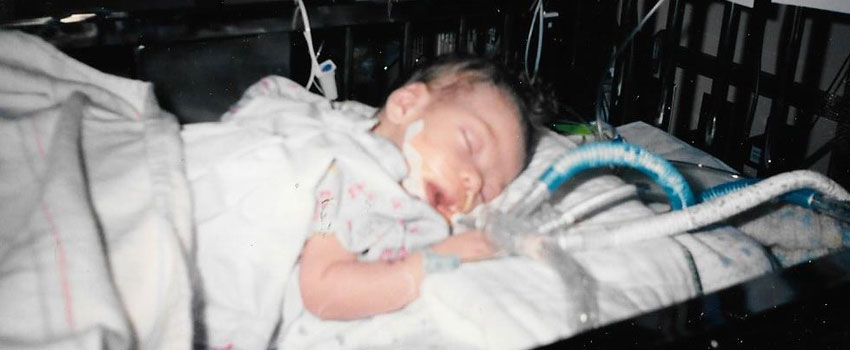

At 4 years old, Sarah Radocha knew exactly what she wanted to be: a newborn intensive care unit (NICU) nurse.
She knew she’d been inspired by her mom, Bobbie, who’d had that job for 16 years at St. Luke’s Boise hospital.
“She would see me go to work, see that I loved my job, loved what I did, and I think that had a big influence,” Bobbie said.
As she got older, Sarah realized it was even more of a calling.
Sarah, now 26, was a NICU baby. She spent nearly two months paralyzed after contracting a rare infection at just 16 days old while at home.
In March 2017, she became a St. Luke’s NICU nurse, just like her mom.
“It was always my goal,” she said. “I had to work hard in school, but it’s just what I always wanted to do.
“Helping babies in a situation like I was, helping the parents, it’s pushed me a lot, but it’s also been so rewarding.”
Her mother recalls sitting on a picnic table at the family’s home north of Eagle, a sunny spot that let her relax with newborn Sarah. Horses galloped nearby and dogs ran around, loving the open space.
On that day in 1994, Sarah’s lips started to turn blue. She wasn’t eating, and there had been periods where she struggled to breathe. A visit to the doctor didn’t turn up anything; Bobbie’s experience told her otherwise.
As Sarah’s 17-year-old sister drove to St. Luke’s, Bobbie made sure Sarah continued to breathe. Once they arrived, a nurse that knew Bobbie got them quickly to the NICU.
The next day, Sarah suffered respiratory arrest and was put on a ventilator. Three days later, she was diagnosed with airborne infantile botulism, which affects fewer than 1,000 babies annually. The bacterial source was never identified, but with farmland and animals all around them, there was no shortage of possibilities.
“It’s pretty amazing to hear about how everything happened, and learning about it, just how unique it was,” Sarah said.
Paralysis quickly set in, and Sarah was put on a ventilator, which she would need for 41 days. Bobbie continued to work, making sure that she was not in the same room as Sarah during her shift and letting colleagues take care of her infant daughter.
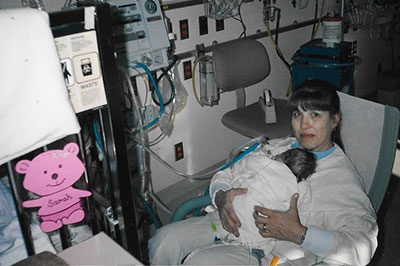
As soon as her work day was over, she spent time with Sarah.
“Some of the nurses would update me, and sometimes it would be something like ‘She’s awake,’ but I’d just say, ‘I’ve got these other babies to take care of,’” Sarah’s mother recalled recently.
“I trusted them, and me hovering would not have helped.
“I have nothing but praise for the knowledge and the skills of the nurses and the doctors in the NICU,” she said. “It’s just amazing. If I hadn’t taken her in, she would have died.”
Joan Hecker, today a lactation educator in the NICU, was one of the nurses that took care of Sarah.
“I remember standing over her isolette,” Hecker said. “We were all worried. She was like family to us. But she had the best of the best looking after her.”
Sarah was taken off the ventilator on Dec. 6 and discharged two weeks later. At home, she had a nasogastric feeding tube until Jan. 15, nearly three months after going to the NICU, when she finally could take a bottle.
Sarah grew up healthy, graduated from Lewis-Clark State College in Lewiston – and returned home to work in the place where she spent those difficult days at the beginning of her life.
“I can hardly talk about it without being emotional – the first day she came to work, I just got misty-eyed,” Hecker said.
“You have to think, ‘It’s a miracle you’re standing in front of me.’”
Now, Sarah can truly understand the feeling her mom, Hecker and others had when she left the NICU.
“Helping parents teach the babies how to eat, seeing them hold the babies for the first time without breathing assistance, those are special moments,” Sarah said.
“We see the whole spectrum, from ones that are in less than a day for low blood sugar, to micro preemies born at 24 weeks. To see them all develop is pretty special.”

All in the family …
One of Sarah Radocha’s co-workers was inspired to work in the newborn intensive care unit (NICU) after her experience, but it was after she had a NICU baby.
Courtney Warner started at St. Luke’s as a surgical nurse. A few months later, after her son Mason was born in March 2013, she was inspired by the work in the NICU to help her son.
Mason was born with gastroschisis, in which a child is born with intestines outside the abdomen. Mason had his first surgery four hours after being born, and another when he was five days old.
“I knew before I had him he would need surgery, and Dr. Jim Vanlooy put me at as much ease as I could be at knowing what was coming,” Warner said. “I thought that was super cool.
“After I had him, thought the staff took phenomenal care at a super difficult time. I thought they did such a good job, I thought, ‘I want to be a part of this.’”
Once back to work, Warner applied to be transferred to the NICU, but the unit wasn’t hiring. She tried again about four years ago, and she got her wish, adding, “I’ll be there forever.”
Every day, Warner still sees her son at what is now her workplace; she passes a photo of Mason regularly in the NICU’s Hall of Hope.
“I love seeing that reminder of why we do what we do when I walk into work every day,” Warner said. “I love that almost all of our babies get better and go home. We almost always have good outcomes.
“We have the best staff.”
About The Author

Dave Southorn works in the Communications and Marketing department at St. Luke's.